Here’s the Lowdown on Birth Control
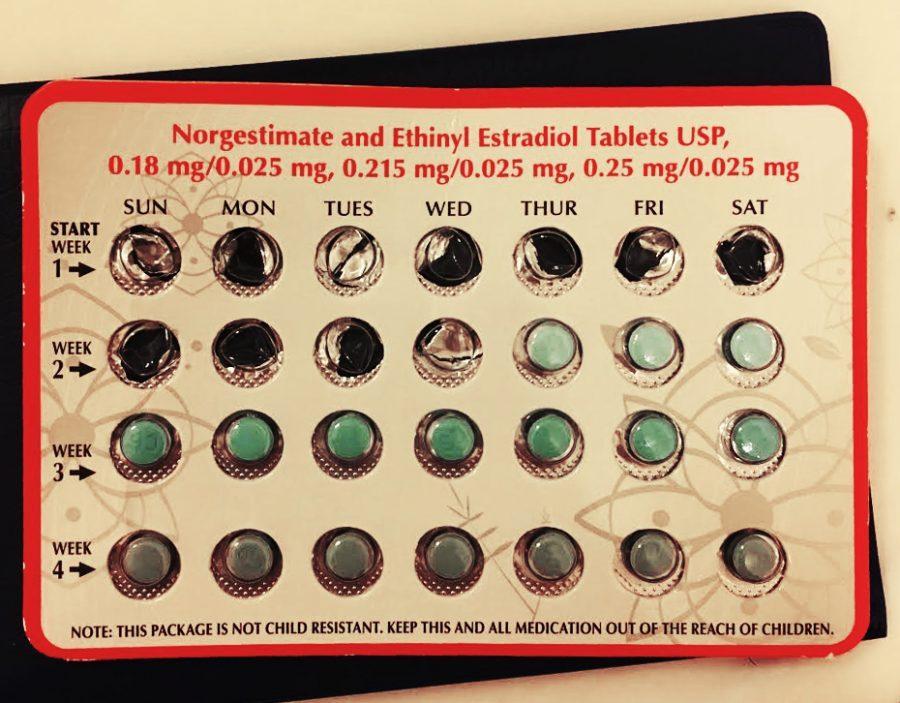
The pill is 99% effective and a popular choice among birth control users.
September 16, 2016
There’s only one way to get pregnant, but fortunately, there are several ways not to. Here’s the low-down on some of the most common forms of birth control, their effectiveness, how they work and most importantly, how you can get them.
Condoms
Effectiveness: 98 percent with perfect use, 82 percent with regular use.
Rubbers: tried and true, they’re the first thing that typically comes to mind at the mention of birth control, and they’re also the only form of birth control that protects against sexually transmitted infections. They’re given out for free basically everywhere on campus: all residence halls, the Student Resource Center, Health Promotion Office, LGBTQ Student Center and Center for Multicultural Education and Programs. However, condoms aren’t foolproof. They can slip or break, so if you’re having sex regularly, and you and your partner have been tested for STIs, you may want to consider an alternative form of contraception.
Birth Control Pills
Effectiveness: 99 percent with perfect use, 91 percent with regular use
The pill is another time-tested form of birth control, containing either progestin or both progestin and estrogen. It works by suppressing ovulation and thickening cervical mucus to keep sperm from reaching an egg. For the pill to work with 99 percent effectiveness, you need to take it at the same time every day. Some people report negative side effects, like spotting, nausea or weight gain; however, there are several different brands of birth control pills, and it may take some experimentation to find the one that’s right for you.
Birth control prescriptions are covered 100 percent at the Student Health Center, and you can obtain a prescription with a quick Well Woman visit at the SHC.
Intrauterine Device (IUD)
Effectiveness: more than 99 percent
These T-shaped devices sit inside the female uterus, with a string extending down through the cervix, and they prevent sperm from reaching an egg. The two most common brands are ParaGard and Mirena: ParaGard is a copper, non-hormonal IUD that lasts for up to 12 years, while Mirena releases progestin and lasts up to 6 years. People who use the ParaGard may notice heavier menstruation, while those who use hormonal IUDs may have lighter periods, or no periods at all. Insertion may be invasive and painful, but on the bright side, this pain pales in comparison to labor.
IUD insertion is only offered at the Student Health Center for those who have NYU Student Health Insurance; the procedure is paid under the outpatient benefit outlined here. For those with other insurance, IUD insertion is offered at Langone’s Women’s Health Free Clinic and at Planned Parenthood’s Margaret Sanger Center.
Implant
Effectiveness: more than 99 percent
A birth control implant is a small rod inserted into a female’s arm. It functions just like birth control pills, preventing ovulation and thickening cervical mucus, but that also means it has the same potential side effects. However, there’s no maintenance involved with the implant, meaning no room for human error, and it lasts up to four years. NYU health insurance coverage for the implant is the same as that for the IUD.
These are many more forms of birth control; these are just the ones with the highest rates of effectiveness and user satisfaction. If none of these are right for you, you may also want to consider female condoms, Depo-Provera shots or birth control patches.
In the event that you do have unprotected sex, emergency contraception (“the morning-after pill” or “Plan B”) is available over-the-counter at the Student Health Center, as well as at any public hospital in the city. Should you become pregnant, abortion services are available under NYU student health insurance.
Note: All statistics on effectiveness are from Planned Parenthood.
Email Abigail Weinberg at [email protected].